In the mid-1970s when I first joined the theology faculty at Notre Dame, I designed undergraduate courses that took up some of the hot issues of the day, including in the field of bio-medical ethics. One topic that I consistently covered was organ transplantation, particularly kidney and heart transplants. The latter received more regular attention in the press because of the symbolic connection of the heart with the center of the self. However, even kidney transplants, in which one human person was harmed in order that a relative (or other patient) might have health restored, required appropriate ethical analysis.Little did I know that over 30 years later I would move from the theoretical to the practical, that I would become a kidney donor myself.
My nephew, Johnny Rorapaugh, was diagnosed at 38 with kidney disease in mid-July of 2006. This meant that he had to quickly move into a regimen of dialysis treatments three times a week for four hours at a time. While dialysis and the accompanying treatment saved his life, the only real remedy for kidney failure is a kidney transplant either from a cadaver or a living donor. The necessity for twice-weekly dialysis is a medical practice that affects dramatically the life of the patient – the tethering to a machine can become a kind of imprisonment. Furthermore, with the passage of time the process becomes progressively less effective.
Because there are 80,000 Americans presently in need of a kidney transplant, the waiting time for either a cadaver or living transplant usually stretches into multiples of years. And because the success rate is twice as high with living donors, the main way to move up quickly on the list is to have a loved one or friend volunteer as a donor.
Johnny was enrolled at the kidney transplant unit at Johns Hopkins Hospital in Baltimore, Maryland (often rated the #1 medical care facility in the country). The medical team was eager to facilitate the surgery if only a volunteer could be found who specified that he or she would only donate if Johnny were the recipient.
At first, at 66-67, years old I thought I would be beyond the acceptable age. After none of the immediate family proved to have the proper blood type and antigen matches, two of my female cousins came forward but, unfortunately, both were disqualified in turn. Then it became apparent that I was, in fact, the best potential candidate (including the age factor). So I began a process of testing that stretched over 6 months, the last stage of which was a full battery of tests (CAT scan, chest x-ray, stress test, blood and urine work, and psychological interview) at Hopkins itself. Once it was clear that I had passed muster, we set the date for the surgery for August 11.
A complication
Then, about 3 weeks before the announced date, I received a call out of the blue from one of the surgeons at Hopkins who introduced a significant complication – would Johnny and I be open to a swap in which a mother-son incompatible pair would be matched with Johnny and me as a compatible pair. At first, I did not know what to say. This would mean that some of the intimate corporal connection would be lost, uncle to nephew. But, after Johnny and I discussed the possibility further, we both recognized that we had the opportunity to help significantly improve (and perhaps save) two lives and not just one. So we quickly and enthusiastically agreed to the swap.
On Monday, August 11, 2008, at Hopkins Johnny received a 33-year old kidney from the son (the primary medical reason for initiating the swap) and a few hours later I donated my 67-year-old kidney to the 61-year-old mother. After 3 days of post-operative recovery, the two donors were discharged (myself included) but not before the four of us met each other for the first time. Bev Bellopatrick had a professional career as a nurse in Colorado. She had come down with diabetes and, as a result, had been on dialysis for 4 2 years. Her plight had become so desperate that a local t.v. station had run a special appeal seeking a donor. Two weeks before learning about the surgery, she had registered in the kidney program at Hopkins. Her son, George who works for United airlines in Denver, had volunteered as a donor if a swap could be worked out.
Johnny and Bev have both been released from the hospital and are well on their way to non-dialysis dependent lives. George and I have both experienced the amazing resiliency of the human body and the special bond that the gift of an organ can bring.
From my first hand experience, the skill of the physicians and nursing staffs at Hopkins is world-class. So are the support structures both prior to and after surgery. Yet, just as amazing, is the fact that all of the basic costs for kidney transplantation (at Hopkins and elsewhere) are covered by federal grants.
In the end, I cannot explain what God had in mind in endowing us with two kidneys when biologically we only need one. ( My own father lived a long and fruitful life with only one kidney). I can only speculate that maybe it was so that we could give one away (when the motivation was strong and circumstances right). The need out there is great. I can only hope and pray that the story of Johnny, me, Bev and George may strike a positive chord with others who have contemplated such a gift.
Father Malloy is president emeritus of Notre Dame.
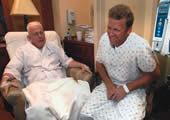
_Photo of Father Malloy and his nephew, John Rorapaugh, by John Long. _